Immunomodulatory Treatments in IVF. Should They Be Used in Cases of Implantation Failure?

When IVF fails, it’s tempting to try anything that promises better odds. But immune treatments like intralipids or IVIG aren’t supported by solid evidence. Studies show they don’t improve implantation or pregnancy rates — and they can carry risks. Instead of turning to experimental immune therapies, IVF care should focus on proven, individualized, evidence-based approaches that truly support success.
📌 What you will learn in this article:
- Why is my body rejecting the embryo?
- What immunological treatments are commonly offered in IVF?
- Do intralipids and IVIG really improve success rates?
- What are the risks and side effects of these immune treatments?
- What do ESHRE and the scientific community recommend?
- The “Haute Couture” Approach: What to Do After Repeated Failures?
Click on the image to watch the video on YouTube.
Why Is My Body Rejecting the Embryo?
Almost every week, I sit across from patients who are drained — physically, emotionally, spiritually. Failed cycles take a toll. And sooner or later, someone asks through tears:
“Doctor… is my body rejecting my baby?” That question hurts. Because behind it is guilt, fear, and the quiet worry that their own body is somehow the enemy. Fertility treatment can feel like an emotional rollercoaster with no seatbelt.
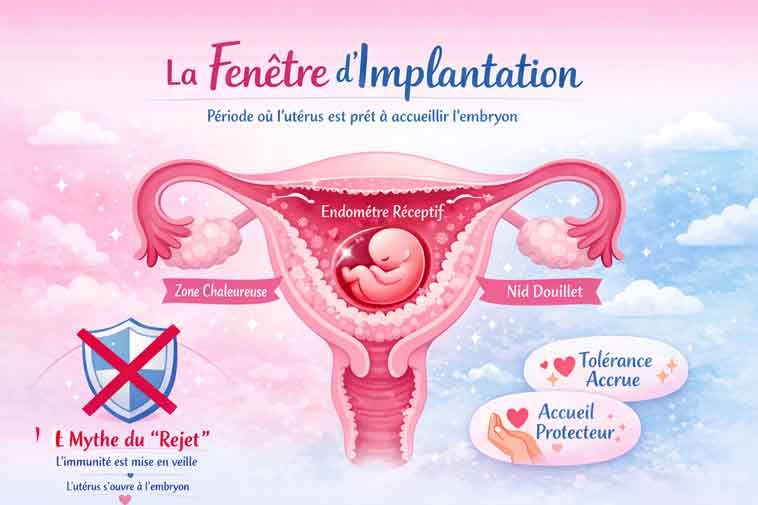
But medicine has to stand on science, not fear. In more than +30 years of practice, I’ve watched countless medical trends rise with great promise — and quietly fade when evidence failed to support them. The idea that we can “manipulate” the immune system to force implantation is one of those trends. The uterus isn’t a fortress under attack. It’s fertile soil. And success isn’t about overpowering the body — it’s about timing and biology. The right seed (a healthy embryo) needs the right conditions and the right moment — the implantation window — to take root.
What Immunological Treatments Are Commonly Offered in IVF?
In more than +30 years of practice — and after helping bring over 10,000 babies into the world — I’ve seen many patients arrive with long lists of treatments they discovered online. The common promise? Calm the immune system, and implantation will happen.
Here’s what that usually involves:
- Intralipids: A fat-based infusion intended to suppress certain immune cells.
- IVIG: Intravenous antibodies designed to modify immune responses.
- PBMC: A procedure where processed white blood cells are placed into the uterus.
- Tacrolimus & Anti-TNF drugs: Strong medications that dampen immune activity.
They may sound sophisticated — even reassuring. But before adding powerful interventions, it’s essential to ask a simple question: Is there solid scientific proof they truly improve outcomes?
Do Intralipids and IVIG Really Improve Success Rates?
Let me be clear: these interventions do not enhance embryo implantation. When it comes to fertility treatment, we must separate hopeful theory from proven results — and the evidence simply doesn’t support immune therapies as a solution.
The evidence speaks for itself. A recent systematic review (Melo et al., 2022) examined multiple studies and concluded that none of these treatments should be recommended.
- Intralipids: So far, there’s no solid, reliable evidence that intralipid infusions improve live birth rates.
- IVIG: The best-quality evidence we have — including a well-designed randomized controlled trial — shows no meaningful benefit.
- Recombinant LIF: This one is especially telling: in clinical research, it led to fewer live births than placebo in the women who received it.
The ESHRE guidelines published in 2023 align with this position. We base our practice on science — and that means we must not make false promises, whether financial or emotional, with treatments that do not work.
What Are the Risks and Side Effects of These Immune Treatments?
As a physician, my job is to protect you. And interfering with the immune system is never a “small” intervention — it’s powerful medicine that should only be used when there’s a clear, proven reason.
Below is a summary of risks documented in the literature (Moffett & Shreeve, 2015; Sfakianoudis et al., 2021):
| Immunological Treatment | Documented Side Effects and Risks |
|---|---|
| Intralipids | Hepatomegaly (enlarged liver), jaundice, thrombocytopenia, fat overload syndrome. |
| IVIG (Immunoglobulins) | Aseptic meningitis, renal failure, thromboembolism, anaphylactic reactions. |
| Anti-TNF | Severe infections, lymphomas, demyelinating diseases, cardiac insufficiency. |
| Tacrolimus | Documented congenital malformations (4% of post-transplant pregnancies). |
In my view, the use of intralipid infusions in IVF exposes patients to hepatic and hematological complications that are entirely avoidable.

What Do ESHRE and the Scientific Community Recommend?
In France, the Haute Autorité de Santé (HAS) takes the same stance. Reproductive medicine, they emphasize, must remain firmly grounded in robust data and the principles of evidence-based medicine.
There’s also an ethical dimension we cannot ignore. Prescribing powerful immunosuppressive treatments to otherwise healthy women — without clear proof of benefit — raises serious concerns. Patient safety, scientific rigor, and medical integrity must always come first.
The “Haute Couture” Approach: What to Do After Repeated Failures?
My philosophy has always been what I call “haute couture” reproductive medicine. No two patients are the same, so why should their treatment be? Instead of applying the same standard protocol to everyone — or adding costly interventions without clear indication — each case deserves careful, individualized analysis.
If you’ve experienced multiple failures, the key is not to blame your body. It’s to identify the real underlying cause.
1. Embryo Quality Embryo selection is fundamental. Advanced technologies, combined with the expertise of a skilled embryology laboratory, are essential to identify the embryos with the highest true implantation potential.
2. The Uterine Environment The uterus must be carefully assessed to rule out the presence of polyps, chronic endometritis — which is treated with antibiotics, not immunosuppressants — or adenomyosis. A healthy environment is essential for implantation.
3. Protocol Personalization Hormonal stimulation should never be “one size fits all.” Dosages must be calibrated with precision — almost surgically — according to each woman’s ovarian reserve, hormonal profile, age, and response to previous cycles. Subtle adjustments can make a meaningful difference.
In the end, success rarely comes from therapeutic escalation or experimental add-ons. It comes from something far less flashy: rigorous science, careful analysis, and authentic human care.
That balance — scientific precision combined with genuine compassion — is often what rekindles hope when standard protocols have fallen short.

FAQ — Your Most Frequently Asked Questions
Why do some clinics offer intralipids if they don’t work?
Because hope sells. When patients are worn down by repeated IVF failures, it can be tempting for some centers to offer something “innovative” or “experimental” — something that feels proactive. Intralipids often fall into that category. They create the impression that more is being done. But here’s the uncomfortable reality: to date, there is no solid scientific evidence showing that intralipids improve pregnancy or live birth rates in IVF. None.
What we do know is that immunomodulatory treatments are not harmless add-ons. They carry real medical risks. And medicine should never be practiced to reassure anxiety, to appear cutting-edge, or to justify higher costs. We prescribe treatments when clear benefit has been demonstrated — not before.
Adding a useless intervention to an otherwise healthy woman is neither good science nor good ethics. It’s our responsibility to protect patients from both false hope and unnecessary harm.
Can the immune system cause recurrent miscarriages?
Yes — but only in very specific, well-defined cases. Certain clearly identified immune conditions, such as antiphospholipid syndrome (APS), can cause recurrent miscarriages. This disorder increases the risk of placental thrombosis and requires targeted treatment. And that treatment has nothing to do with intralipids.
In APS, management is based on anticoagulants such as heparin and low-dose aspirin — validated therapies with demonstrated efficacy. Prescribing heavy immunomodulators without a precise diagnosis, however, has no solid scientific basis. In medicine, we treat an identified cause — not a vague hypothesis.
Are PBMC cells useful for thickening the endometrium?
No. Current scientific data show no meaningful benefit. A recent review (Melo et al., 2022) classifies the evidence supporting intrauterine PBMC use as being of very low quality — meaning available results are insufficient to conclude any real efficacy. As a result, their use is not recommended by ESHRE. In reproductive medicine, when a treatment rests on weak or insufficient evidence, caution must prevail. The absence of solid proof is not a minor detail — it is a warning sign.
How does Dr. Aksoy manage implantation failure?
I take a personalized clinical approach — a true “haute couture” fertility medicine. When facing repeated implantation failures, I do not multiply experimental treatments. I start by looking for the real cause.
My strategy rests on three pillars:
- preimplantation genetic testing (PGT-A) to assess embryo quality,
- detailed hysteroscopy to precisely analyze the uterine cavity,
- and personalized hormonal optimization, carefully adjusted to each patient.
The goal is not to add more options — it is to provide solutions grounded in science. Unproven treatments have no place in this approach. Because in reproductive medicine, rigor and personalization make all the difference.
Can I get pregnant after 3 failed IVF cycles?
Yes, it is possible. Three failures do not mean the journey is over. Many patients achieve pregnancy after multiple attempts, especially when a precise medical diagnosis replaces repeated blind trials. Often, the difference lies not in “doing more,” but in doing better: understanding embryo quality, evaluating the uterine environment, and fine-tuning hormonal stimulation. A second expert medical opinion can sometimes completely change the strategy — and with it, the outcome. After several failures, the answer is not to give up — it is to reassess intelligently.
Legal Notice
Date of last medical review: February 22, 2026.
This article was written and medically validated by Dr. Senai Aksoy (Obstetrician-Gynecologist, Specialist in Reproductive Medicine) for strictly informational purposes. Each patient is unique and IVF outcomes vary according to many medical factors. This content does not replace a medical consultation. Please always consult your physician regarding your personal situation.
© Assoc. Prof. Dr. Senai Aksoy — All rights reserved.
The content has been created by Dr. Senai Aksoy and medically approved.

